My twenty-fifth birthday ended up becoming a lot more memorable than I thought it would be. Besides the ability to rent a car without paying an exorbitant extra fee (which would have been useful when renting an expensive minivan for a weekend in Cedar Point) – the “youth tax,” there’s not much else that comes to mind about officially being in ones “mid twenties.” But when I started having strange back pains early last week, I didn’t think I would end up spending last night in the hospital.
I’m no stranger to back pains, even ones that last for a couple days. But these ones were different – they didn’t seem to be caused by lying, standing, sitting, or slouching in a particular way. It was kind of a dull ache that was focused specifically on my lower left shoulder blade, and over the next few days, i found that its intensity would increase while walking, running, biking, or doing anything that wasn’t sitting perfectly still. I noticed at work that I was getting a bit out of breath while climbing the stairs (and since the elevator up to the 8th floor has been out all summer and I have numerous computers to configure up there, I have been using those stairs pretty constantly). After returning my desk, though, the pain would fade to its general dull ache. At its worse, it felt like a needle being jammed into my lower back that would slowly radiate pain up into my upper shoulder – but always on my left side. At my parents’ house for my birthday this past weekend, my family urged me to look into seeing a doctor. But I kept hoping it would just go away.
Besides taking a sick day off of work and sitting with an ice pack occasionally at home, I didn’t do anything about it until a week later, when I finally called the doctor this past Monday. I imagined at best it was pleurisy, at worse it was a very slow-acting heart attack. Most likely it was just a deep muscle ache that a back rub couldn’t reach. But why was I short of breath?
Although I wouldn’t be able to use my new “primary care provider” due to a 9 month long waiting list for an introductory appointment (ah, so that’s why people make fun of HMOs) they got me into an appointment on Thursday, although they said that if it was an emergency of course they wanted me to come in right away. I told them that if I had made it this long without seeing anyone, I probably wasn’t going to keel over.
At yesterday’s appointment with UW Health, they shuttled me between the x-ray room and the on-call doctor. After explaining to a nurse and Dr Greg my entire family medical history – a downside of switching to my own insurance with a different provider than my parents – Greg listened to my lungs through his stethescope several times. He reported that my left one sounded different, and sent me down for the first set of xrays. He looked at them, then sent me down again to do more, this time while exhaling my breath entirely outwards so that they could see where my lungs were. I could tell what they were assuming, and it didn’t look good.
After I returned to the exam room, Greg sat me down with the xrays and showed how the upper edge of my left lung had detached itself from the pleura and there was now a pocket of air pushing its way around between my lung and the inside of my body cavity. The bubble would shift itself around as I moved about, and would probably explain why I felt most comfortable while lying down. He transferred me over to a pulmonologist in another building who explained things even more clearly – apparently, I am the perfect demographic to get this injury, which is called primary spontaneous pneumothorax, PSP, or more colloquially – a partially collapsed lung. Sufferers are usually tall, skinny, male, and between 20 and 30 – how fitting that I had just passed my mid-twentieth birthday. “Basically, people who look like Abraham Lincoln,” joked my specialist, Dr. Cole. He further explained that it was because I was tall and skinny that my lungs had a lot of surface area on them, and a lot of weight pulling them downwards – apparently, the left one had succumbed to gravity and pulled away from the upper pleura.
I had several options, he continued. I could either wait and see how quickly it would heal – as it was only a 3% partial collapse, he figured that I should heal up nicely. More drastic measures would be to stick a needle into me and pull the lung wall back out again, taking the air with it, or keep a quarter-inch thick chest tube in my side for a week to siphon out the air. But those would be overreacting, he concluded. Because I have a trip to Costa Rica planned for next month, however, I asked him if there was anything else I should worry about.
He got a little more somber and told me that possible health complications could result from the air pressure change in a flight, and that although the risk was small in my case, it could be a big problem if that air pocket swelled while in reduced air pressure. Some airlines don’t even let you fly unless you can tell them you haven’t had a pneumothorax for 6 weeks or longer. He said that if we could get it done with 2 weeks of safe period before the flight, he’d think I was safe.
Two weeks from today is when I fly out. Well then, our fastest and least invasive procedure is treating you overnight on 100% oxygen, he told me. It seemed suspiciously easy to me – lie in an air conditioned hospital room with a mask on? How could that possibly remove air trapped in my chest? Because the air in that pocket is plain atmospheric air, Dr Cole explained. Pure oxygen in your lungs will cause the nitrogen-rich regular air molecules to diffuse through the lining and back into your lungs, where it can be exhaled normally. Then your lung will be able to press up against the pleura again – and then hopefully reseal itself there permanently.
I checked myself back in later that evening, and was escorted up to my room by an admittance nurse. Over the course of the next hour, three different women visited – two with badges that said CNA, and one RN. No oxygen during that entire time, so I just read my book and snacked on my jug of peanuts I’d brought with me. But eventually someone came in with a mask in a sealed plastic bag and a long tube, which was plugged into a green faucet-looking device that came out of the wall. Gone are the days of individual oxygen tanks, apparently. They plugged it in, plugged me into it, and cranked up the output to 15 liters per minute. Considering that the normal flow rate for senior citizens on oxygen is about 2 LPM, the attendent CNAs must have wondered what on earth could be wrong with me that I would need that much oxygen.
I amused myself for a few minutes watching little rubber output gasket on the side flutter as I exhaled, but the constant hissing noise of the system got tiresome quickly (I wish that I had bothered to check for earplugs sooner; I found some on the nightstand in a little bag the next morning). The nurses cycled around through shifts, each time coming in and checking my pulse and oxygen count with a little device that clipped onto my index finger, which without making any sort of cut in me, was able to measure oxygen percentages in my blood. I had been at 96 that morning, but after being on pure oxygen for a few hours, I hit 100 each time.
The oxygen mask had a strange little bag under it, like a wattle on a goat, that didn’t seem to do anything except be filled with air at all times. It’s not like it was needed, though – the hose kept an unceasing supply of air roaring at my nose and mouth at all times. The bag constantly got in the way though as I shifted and tried to get comfortable in the bed as midnight drew near; it’s difficult to lie on your side with a tube coming off of your mouth and an air-filled bag trying to sit under your chin. I licked my lips occasionally; I could feel them getting chapped with the gale-force winds blowing at them.
I woke up somewhere around 4 in the morning when a nurse named Walter with a Russian sounding accent came in to check my vitals yet again, and he rolled down the shade facing the east (I could see the capital rotunda from my window, twinkling cheerfully at me in the darkness) and whispered to me that otherwise, I would be blinded by the morning sunlight in a few hours. The next thing I remember is my alarm waking me for work at 6:45, causing me to snap my head upright and the airbag to pop up and bap me playfully in the eye. It looks like you can sleep through anything if you get accustomed to it, even a hissing, oddly-constructed air mask.
My morning x-rays followed some hours later as the sun rose. It was time for the doctors to see if the pneumothorax had indeed withdrawn into the comforting fold of my lungs yet again. I wasn’t willing to bet anything, yet – my back always hurts on strange new (hard) beds like this one, so I couldn’t tell if I felt any different yet. And the nurses certainly weren’t assisting in my wish to see if I was still in pain – I was carefully bundled out of bed into a wheelchair, with a blanket wrapped around me, as nurse Ginny soothingly told me that she would disconnect my air just for a second and then she quickly attached it to a portable air tank on the wheelchair. None of the nurses seemed to understand that I wasn’t suffering from oxygen deprivation and that I wouldn’t turn blue and die if I was off the feed for a minute – they just saw the high flow rate and assumed that I should be treated like delicate glass.
I was carefully wheeled down the hall a “transport” nurse, to the elevator, and down to the x-ray room, where the x-ray technician told me I didn’t need to remove my nightshirt or my oxygen mask; a far cry from the torso disrobing that was ordered the previous morning. Once again, it seemed like I was being treated very gingerly. I wasn’t sure if he knew that the only way to see my small pneumothorax was to take the x-ray while exhaling fully; after all, the previous technician hadn’t apparently known it on the first try yesterday. So I did so without telling him (even though he told me to inhale, like most x-ray techs do) as I hoped it would be helpful to Dr Cole or whomever would look at the scans. Then I was carefully eased backwards into my chair again (the whole process had required me moving all of a foot) and a second transport nurse took me back to the room. She asked me in a slow, over-annuniciated voice if I was a student at the UW. With some amusement, I told her that I was a computer consultant and technician for the UW. “Oh!” she replied with a note of some surprise. “Well that must be a very good job for a smart young man like you!”
It’s interesting how one’s attitude towards people change if they seem helpless, ill, and needy. To the eyes of the many nurses who had been attending to me for hours, I was a skinny, frail looking guy with glasses in pajamas who had been wearing an oxygen mask all night and needed chest x-rays. They spoke in a very cheerful, evenly-paced upbeat tone without fail. Once I asked about whether their computers were running Epic’s medical software, or mentioned my work as a consultant for another UW department, the tone changed a bit and then they would talk to me normally – or at least, until they cycled out again and a new nurse arrived and I needed to repeat the process over again. I felt silly being babied and assisted about. I had gone 9 days with a partially collapsed lung and I knew I could handle it – so I didn’t feel like I should be accepting their professional kindness. I didn’t want to be a burden.
After returning to my bed and my wall-based oxygen source for another half an hour, Dr Cole came in with the good news – the pneumothorax had disappeared, and my x-ray looked normal – his plan had worked. My back was still stiff enough (probably in part from the lack of my own personal locomotion!) that I couldn’t tell if I felt better or not, but I was greatly cheered that things looked normal from his perspective. He confirmed his guess with a quick listen to my lungs again with his stethescope, and I could feel the tension and relief ebb out of me – I could go back to normal.
But wait, he cautioned – I still want you to come back next week for a followup. Oh. Well, of course that makes sense. “And,” he continued, “we’ll need to keep an eye on your lungs. No lifting anything over 20 pounds for 2-4 weeks. Also, you have a 33% chance of developing a second pneumothorax, now that you’ve had one.” I asked him what the odds were for the general population. 18 in 100,000 he replied. So my odds of a relapse have increased significantly. And if I were to get a second one, my odds of a third one would increase to 80%. “At that point, there is a surgery that we would recommend after the second to irritate the pleura of the lungs with some powder, which would then develop a sticky blood clot along the edges which has a 98% success rate at making your lung stick in place, permanently.”
I took off the breath mask and shut off the oxygen myself after Dr Cole left. The room felt very quiet without the constant hissing sound I’d grown accustomed to for the past 15 hours, and it took me an hour to become re-acclimated to working hard to breath again in the regular air. I packed my things and prepared to walk back to work, but the nurse told me that walking a mile seemed like too much stress for me because it was “very hot outside.” She wanted me to take a taxi but in the end we compromised with the bus system.
It feels really good to be free of that twinging lung pain (and have it replaced with good old familiar vertebral back pain again) but I guess it was a wake up call for me – they never tell thin young people to be on the lookout for collapsed lungs. In comparison with heart disease and diabetes, I guess I’ll be thankful that there’s comparably less things that affect people with my body type. Except, as I told my boss, the fact that people like me will be the first ones to succumb after the next ice age due to the lack of fat storage!
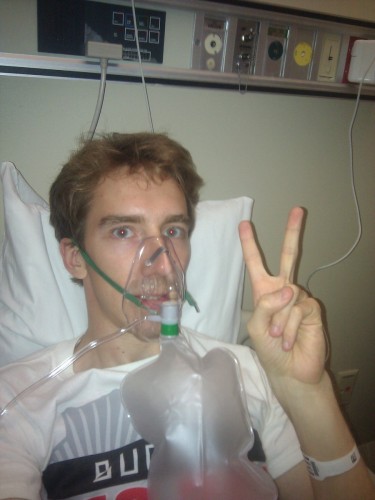


We’d better hope that ice age stays away for awhile!
Another ice age doesn’t seem like where we’re headed at the moment, does it, Andy!
Good article on your brief sojourn in the UW Hospital system, Zach! I thought it was a bit scary that in two of three cases, the x-ray techs either weren’t informed what sort of view Doctors Greg or Cole were seeking (ie, taken on full exhalation), or chose to ignore those instructions. Fortunately, you were sufficiently on-the-ball for the third x-ray that you knew what to do although instructed to do the opposite!
Salamtak! Glad to read about your travels again. We’re stateside for a few months so if you feel like hopping over the great lake, let us know!
Um Tulip